TABLE OF CONTENTS
- Introduction
- Pop-up alerts on record retrieval
- Templates for consultations
- Reviewing patients with overdue tests
- High risk drugs - Sending reminder notifications in bulk
- Annual Monitoring
- Annual Monitoring | Other by Accessibility
- Removing patients from monitoring
- Frequency of monitoring
- Locally Commissioned Services (LCS)
Introduction
Ardens offers comprehensive drug monitoring services to ensure the appropriate testing is conducted for medications such as ACE inhibitors, anticoagulants, DMARDs and others.
Further information:
Summary of the medications and the associated monitoring tests
Information for the monitoring of sulfasalazine
Pop-up alerts on record retrieval
Upon accessing a patient's record, a pop-up will appear if the patient is prescribed a high risk drug (e.g. a DMARD) that has associated overdue tests and is under primary care monitoring. The overdue time interval is established based on the maximum recommended duration for monitoring when the patient is stable on their medication, for example, 12 weeks. It is important to note that the patient may necessitate more frequent testing than this interval.
To deactivate these pop-up alerts, navigate to:
Setup > Workflow Support > Protocols
In the left hand pane, open up Ardens > Pop Ups and untick the blue tick next to 'Prescribing Monitoring - High Risk Pop Up Warning'
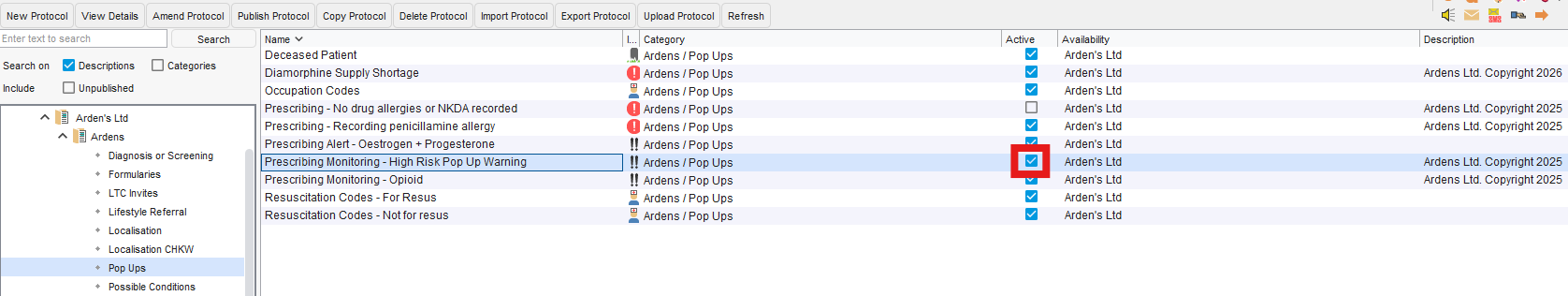
⚠️Please Note: Disabling these pop-ups will remove them for all patients, meaning no drug monitoring reminders will be displayed. Please only proceed if you have alternative systems in place to ensure drug monitoring is maintained.
Templates for consultations
To access the drug monitoring templates, navigate to Auto-consultation > ardens DRUG MONITORING. If a patient is prescribed a DMARD or an anticoagulant, an
If the medication falls under shared care, this can be indicated at the top of the template. If this section is left blank, it will be assumed that monitoring is conducted primary care. As there is only one ‘High Risk Drug Monitoring – Primary Care’ code, it is presumed that if a patient is on two or more high-risk drugs, the monitoring will be consistent across each drug. For guidance on recording hospital medications, please refer to our support article.
The template also contains information regarding required tests and warning thresholds. To view previous notes, click in the free text notes box, these will be displayed on the right-side of the template.

Reviewing patients with overdue tests
To review patients on specific medications with overdue tests, navigate to:
Clinical Reporting > Ardens > Prescribing > Monitoring > Drugs | (Annual, Anticoagulants, DMARDS, HRD).
Here, you can locate the reports for the medication of interest, run the report and subsequently review the patients record. Medications that necessitate monitoring more frequently than annually are classified as high-risk drugs for reporting purposes and are located in the HRD folder, with the exception of anticoagulants or DMARDs which have their own folder.

High risk drugs - Sending reminder notifications in bulk
Reports have been created to identify all patients prescribed a high risk drug that require a blood test.
To locate these reports, navigate to:
Clinical Reporting > Ardens > Prescribing | Monitoring > 1 High risk monitoring | Primary Care reminders
The first set of reports will find patients who are due their blood tests within the next 2 weeks allowing you to be proactive.

This report finds all patients whose test are due soon:
0 Reminder: All ?Send reminder as tests due soon + no 1st reminder in last 3m
The following reports contain all of the patients found in the above report but separated by those you can either notify by Email, Post or SMS.
0 Reminder: Email
0 Reminder: Post
0 Reminder: SMS
Run the required reports and either use the SystmOne Communications Annexe to send messages in bulk, or export the list of patients to Excel if using third party messaging software.
The other sets of reports are to send reminders to patients who are now overdue their blood tests.

This report finds all patients whose tests are overdue:
1st Reminder Due: All ?Send 1st reminder as overdue + no reminder in last 3m (add XaXwg)
The following reports contain all of the patients found in the above report but separated by those you can either notify by Email, Post or SMS.
1st Reminder Due: Email
1st Reminder Due: Post
1st Reminder Due: SMS
Run the required reports and either use the SystmOne Communications Annexe to send messages in bulk, or export the list of patients to Excel if using third party messaging software.
Important:
Once the 1st reminder has been sent, add the code in bulk shown in the title of the report (XaXwg - Medication monitoring first letter sent).
Any patients from the above reports who have not completed their blood tests within one month, will be moved to 2nd Reminder Due reports. You can then send them a further reminder and add the code in bulk shown in the title of the report (XaXwh - Medication monitoring second letter sent).
Repeat the process for 3rd Reminder Due.
Annual Monitoring

Annual Monitoring | Has QOF LTC
Annual Monitoring | Has QOF or Best Practice LTC
Patients that are due annual blood tests, for example, steroids or thyroid medications, and also has a chronic illness.
These patients would have a condition outlined in the QOF contract and/or conditions that fall under Best Practice guidelines.
Use these reports if you DO NOT use the Ardens Long-Term Condition (LTC) recall system.
You should also use Annual Monitoring | No QOF LTC to ensure you capture the full population of patients who require bloods tests. These reports look at all other patients on medications requiring annual monitoring that do not form part of the QOF contract.
If you do use the Ardens LTC recall system, these reports can be ignored as this population of patients are covered within that system.
Annual Monitoring | No QOF LTC
Annual Monitoring | No QOF or Best Practice
These reports identify patients prescribed medications that necessitate an annual review. However, these patients fall outside the scope of the QOF contract and Best Practice guidance. Consequently, the Ardens Long-Term Condition (LTC) recall system will not include these patients. It is essential to utilise these reports to ensure all patients due for blood test are accounted for.
Annual Monitoring | Other by Accessibility
You will also need to use these reports to capture patients who reside in a care home, are housebound or are listed in the dementia, learning disability or end-of-life registers.

Removing patients from monitoring
Patients can be removed from monitoring by stopping the repeat medication, end the acute or by coding the patient with
- For drugs needing more frequent monitoring than annual, that aren't anticoagulants or DMARDS: High risk drug monitoring - secondary care (205811000000106)
- For anticoagulants: Anticoagulation monitoring in secondary care (199761000000102)
- For DMARDs: Disease modifying antirheumatic drug monitored in secondary care (494341000000104)
The relevant code can be found on the corresponding drug monitoring templates.
As an additional safety measure to capture patients who are taking a medication being issued on acute rather than on repeat, we also look for issues of a medication with an end date after today. The exceptions to this are anticoagulants, corticosteroids and azithromycin as these are often prescribed for short courses.
NB As drug monitoring carried out by secondary care at some point generally becomes the responsibility of primary care, the secondary care monitoring code above has to be reapplied every 12 months.
Frequency of monitoring
The interval for Ardens drug monitoring blood tests adhere strictly to national guidelines and cannot be modified by individual practices for local areas. The link provided at the beginning of this article contains a spreadsheet detailing the resources that govern the blood tests and the recommended intervals.
The primary sources for these guidelines typically include the British National Formulary (BNF), National Institute for Health and Care Excellence (NICE), Specialist Pharmacy Service or specialised organisations such as the British Society of Gastroenterology. In instances where national guidance specifies to 'monitor regularly', such recommendations are not included in our reports to avoid introducing subjective interpretations regarding timeframes.
Certain medications have national guidelines that permit extended monitoring intervals for stable patients. For instance, lithium, tacrolimus and ciclosporin may have their monitoring frequency adjusted accordingly. The monitoring templates for these specific medications include a section where codes can be added simultaneously to modify the frequency of invitations.

For patients requiring increased monitoring frequency for specific medications, it is advisable to establish an additional recall on an individual basis.
Locally Commissioned Services (LCS)
A variety of reports are available to fulfill any contractual obligations. These reports can be accessed by navigating to:
Clinical Reporting > Ardens > Contracts | 20xx xx | Local Contracts ....

